Gaya (Bihar): Married early, Premlata Devi had had four children by the time she was 24 years old–a boy and three girls. A homemaker from Tikari block in southern Bihar’s Gaya district, she had had a copper intrauterine device (IUD, the most common brand name being Copper-T) inserted for contraception after the birth of her second child.

Six years later, she had got it removed because of abdominal pains and increased uterine bleeding, both known side-effects of the device. “I no longer want to use Copper-T,” she said.
After the removal of the IUD, Premlata Devi went on to have two more children that she had not planned for. Neither she nor her husband know of alternative methods of contraception, she said. And the health workers, who under the National Health Mission are supposed to counsel women like her, never did show up.
Stories like these are common in Bihar, India’s fifth poorest state and third most populous, with India’s highest total fertility rate (TFR)–3.4 children per woman, according to 2015-16 government data, the latest available. This TFR exceeds that of India’s most populous states: Uttar Pradesh (2.74) and Maharashtra (1.87). The national average is 2.18. (Sikkim and Kerala had the lowest TFR for 2015-16: 1.17.)
In roughly five years, or by 2024, the population of India is expected to surpass that of China, according to a 2017 United Nations (UN) projection. China’s population will peak at 1.44 billion in 2029 and then start declining.
Due to what is called population momentum–a higher proportion of people in the reproductive age group–as well as higher life expectancy, India’s population will only peak in the 2060s, before it starts to decline, according to current estimates.
However, Indian fertility rates are declining, and some of these estimates are revised constantly. For example, according to earlier UN estimates, India was to overtake China in 2022. Ten years ago, India had a TFR of 2.68; today, according to the National Family Health Survey 4 (NFHS 2015-16), out of the 36 states and union territories (UTs), only four–Uttar Pradesh (UP), Bihar, Meghalaya and Nagaland–have a TFR more than or equal to 2.68.
Yet, as many as 12 states have a TFR above 2.1, termed the replacement-level rate, at which the population remains constant.
In 2011, Bihar’s population was close to that of the Philippines–the 13th most populous country in the world today. Of Bihar’s 38 districts, 36 report high fertility rates, including Gaya.
To understand why India’s family planning programme launched in 1952, ahead of many other nations, has failed in the state, IndiaSpend conducted a survey among 900 women in Gaya and Patna districts between December 2017 and April 2018.
In this first part of the series, we look at patterns of contraceptive use and awareness among women in Bihar. In the second part, we will examine social factors that cripple the state’s family planning efforts. The series will also focus on unmarried women and adolescents, who are normally not considered in studies that deal with the unmet need for contraception.
We found that while 94% of sexually active women aged 15-49 knew of at least one of the eight contraceptive methods in use, only one in five (20.1%) were currently using any. More unmarried, sexually active women use contraceptives (42%) than married ones (27%), and education increased women’s awareness of contraception.
Fear of side-effects
Given the widespread awareness about contraception in Bihar, why is contraceptive use so low?
The biggest reason, our survey suggested, was a fear of side-effects (15%). This was followed by the desire to conceive (11.7%), general disinclination to use contraceptives (8%) and opposition from partners (7.8%). (The other reasons included lack of access, lack of knowledge, and religious objections.)
The burden of contraception also lay almost entirely on women.
Why No Contraceptive Use
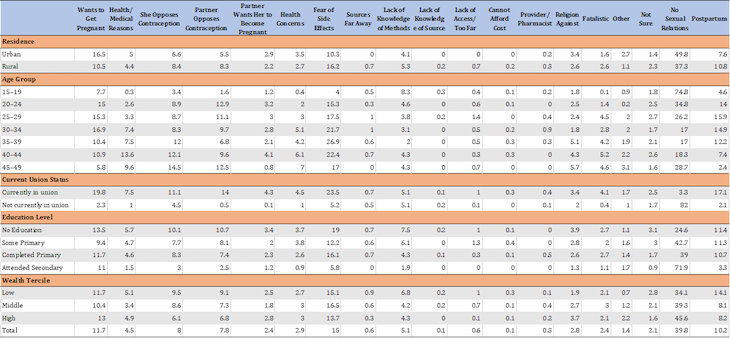
Source: IndiaSpend survey.
Contraception use drops
Over 10 years to 2015-16, the use of any method of contraception among married women in Bihar dropped 10 percentage points to 24%, making it the lowest among all Indian states, according to NHFS-4. The national average is 54%; Punjab fares best (76%), followed by West Bengal (71%) and Chandigarh (74%).
High fertility among women can lead to increased risks of pregnancy-related death (maternal mortality) and illness (morbidity), according to the United Nations. Apart from increasing the population, women with several children find fewer opportunities to improve their social and economic status, making it difficult for them to rise out of poverty. On an average, societies with high fertility demand more services from their governments.
The method most preferred by the women we interviewed was the copper IUD, used by 4% of sexually active women. Of all the sterilisation procedures conducted in Bihar in 2017, 98.9% were on women, according to 2017-18 data from the Health Management Information System.

Female sterilisation was the most common method of contraception used in India, as per a Lancet study. But one in three women in the country also lacked access to contraceptive methods, the study added.

More contraceptive use among unmarried, sexually active women
Bihar’s TFR has always been higher than India’s, and has declined continuously over the years, falling from 4 in 2005-06 to 3.7 in 2011 and to 3.4 in 2015-16.
As we mentioned earlier, of Bihar’s 38 districts, 36 were rated high-fertility districts, according to the Centre’s Mission Parivar Vikas programme. Patna and Arwal districts are the exceptions.
Launched in November 2016, the programme aims to reduce the TFR in 135 districts to the replacement level of 2.1 by 2025, the Hindustan Times reported in November 2017. Replacement-level fertility reflects the average number of children a woman must have to keep the population constant.
Premlata Devi’s district, Gaya, had the third highest percentage of married women in Bihar using any method of contraception–36% in 2015-16, according to the NFHS data. But this was 18 percentage points lower than India’s average of 54% in 2015-16.
The low use of contraception is despite high awareness, we found.
Around 94% of all surveyed women (and 97.8% of married women) in Gaya knew about the existence of at least one of eight methods of contraception, our survey showed. This included traditional and modern methods.
We found that contraceptive usage was more widespread among women who were unmarried and sexually active (42%) than among those who were married (27%). In terms of contraceptives preferred, unmarried women showed a preference for the contraceptive pill (11.2%) while married women preferred the copper IUD (8.6%).
More education = greater awareness of contraceptives
The survey group was divided into two: Women in any form of sexual relationship between ages 15-49, and women who were generally sexually active.
Awareness of modern methods, we found, was higher–94.2% of surveyed women knew of modern methods (condoms, IUDs, etc.), and 46.2% of only traditional methods (withdrawal, breastfeeding).
Of the women surveyed in Gaya, 20% were using some form of contraception; 15% of them were using modern methods. Reasons for low usage included the fear of side-effects and the desire to get pregnant.
| Methods Of Contraception | |
|---|---|
| Traditional Methods of Contraception | Include breastfeeding, withdrawal by men |
| Modern Methods of Contraception | Include female and male sterilisation, the contraceptive pill, intrauterine device (IUD), post-partum IUD (PPIUD, injectables, male and female condoms, and emergency contraception |
Source: IndiaSpend primary research
Data collected during the survey showed that in general, women who lived in cities, had attended secondary school and were in some form of “union” with a sexual partner or husband were more aware of at least one of the eight contraceptive methods.

Among married women, 27.1% were using contraception during the survey period. When compared to the NFHS data for 2015-16, this represented a fall of eight percentage points over two years.

Education also meant more use of family planning devices
As we said earlier, married women showed lower use of contraception compared to unmarried sexually active women. Also, there was greater use of contraception among women who had completed their primary education and attended secondary school. They preferred modern.

The use of contraception among Indians, particularly modern methods, reduced between 2005-06 and 2015-16 due to reasons including unavailability of preferred methods and men’s reluctance, IndiaSpend reported in August 2016.
A later study had shown that over eight years to 2016, contraceptive use in India had dropped 35%, IndiaSpend reported in February 2017. Male sterilisation rates had also dropped to 0.3% from 1% over 10 years to 2015-16.
Among men in Bihar, the use of condoms fell more than a percentage point from 2.3% to 1%; the percentage of men who adopted male sterilisation dropped to nil from 0.6% in 2005-06, as per NFHS 4 data.
Some men believe condoms reduce sexual pleasure and vasectomies rob them of virility, IndiaSpend reported in February 2017. Though vasectomies (male sterilisation) are a quicker, safer and healthier option, they remain an unpopular method around the world. With female sterilisation, there is a small risk of internal bleeding, infection or even an ectopic pregnancy (fertilised egg growing outside the womb), according to the National Health Service of the United Kingdom.
Copper-T most popular method
Medical professionals recommend condoms and vasectomies and, for women, oral pills and IUDs, IndiaSpend reported in February 2017.
Of the 20% of women using contraception in Gaya, the popularity of the eight methods worked out (see table).
The contraceptive method preferred by all women in Gaya was the Copper-T, with 4% of them currently using that method. The second most used was the traditional method of men withdrawing, at 2.8%. Among married women, the preferred method was the Copper-T, with 8.6% of them opting for that method, followed by the contraceptive pill at 4.8%.
In our sample districts, we found that unmarried women’s preferred method was the pill (11.2%), followed by the IUD (9.4%). Their level of education and residence were other determining factors–women living in cities and those who had completed primary education and attended secondary school reported higher percentages of contraceptive use.
The relationship between wealth and contraceptive use was not clear, but women in the higher wealth categories showed higher percentages of contraceptive use.
This is the first of a two-part series.
Next: If Women Could Decide, Bihar Wouldn’t Have A Population Crisis
(Das is a programme policy manager at the International Growth Centre India. He has a Master of Research degree in social policy from the London School of Economics and an MA in development studies from the Institute of Development Studies at the University of Sussex.)
Courtesy: India Spend
